We don’t talk enough about…how little most people know about health and care
Anastasia Knox explains why we need to talk more about how little most people know about health and care, and the impact of this lack of knowledge on relationships, communications and change in the NHS.
The diagram below was drawn by a focus group participant. I had asked everyone to draw a picture of the health and social care system. This is a fairly representative example of what I got back.
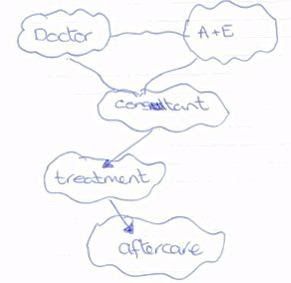
This diagram shows two things. Firstly, although the NHS feels very familiar to many people, their understanding of the ‘system’ is very limited. Most of the people I speak to have little understanding of how different parts of the system work together, the range of work it delivers or how decisions are taken. And, frankly, they have very little interest in these things.
The second point illustrated by this diagram is that, while understanding of the NHS is low, it is miles ahead of most people’s conception of the social care system – you will note the complete absence of the latter in the diagram.
In our research, many people struggle to define what social care is, or the services it provides, much less give an account of how it differs from the NHS, or how it is accessed or funded. There are some indications that levels of awareness are beginning to rise – but not enough yet to make a difference at an overall level.
Why lack of knowledge matters
- Firstly, it has fundamental implications for people’s relationships with health and care services. If people do not understand the systems and what they do (and do not) deliver, then they stand little chance of understanding what their rights and responsibilities are as service users. This is perhaps most vividly illustrated by a woman in a focus group I ran with informal carers. She had cared for both her parents at the end of their lives. After her father died, someone said to her that she should have applied for support from the social care system. For this woman, her lack of knowledge of the system – she had never heard the phrase social care previously – had a direct and negative impact on her quality of life.
- Secondly, it has implications for communications. In the case of the NHS, it means that talking about integrated care systems, or whatever the latest hot topic is, will only work if we avoid assuming knowledge and root the conversation in the issue that ultimately matters most to people – what it means for their care. For social care, the discussion needs to begin with an explanation of the system, including that it is not free at the point of use for most. The challenge here is that the shock of learning more about the system often provokes considerable frustration, and derails the wider conversation.
- Finally, in the case of the NHS, the lack of understanding contributes, at least in part, to a widespread aversion among the public to change. If there are only two ways into the system (your GP and the local A&E) then closing the A&E department – whatever its shortcomings – is a pretty scary prospect, especially given current issues with GP access.
Only once we have understood the gap that exists between many members of the public and those within the system will we be able to design, deliver and communicate services that meet people’s needs.
People’s starting point on the health and social care systems has real implications both for how they behave as service users, and for those working to improve health and care for the benefit of the public as a whole. Only once we have understood the gap that exists between many members of the public and those within the system will we be able to design, deliver and communicate services that meet people’s needs.
This understanding will also enable us to empower service users to make the most of those services, helping people like the lady in my focus group to access the care and support they deserve.
Anastasia Knox is an associate partner at BritainThinks, leading on their health practice with clients including NHS England, Abbott, Age UK and the Health Foundation. Anastasia has written on health issues for the Guardian, the Health Service Journal and the BMJ.
This topic will be discussed at our Super Melting Pot on 16-17 January, where we will be exploring the things that we don’t talk nearly enough about.
 Anastasia Knox14 January 2020
Anastasia Knox14 January 2020

Comments